How Prediabetes Develops into Type 2 Diabetes?
- admin
- October 28, 2024
- 9:33 am
- No Comments

Have you ever wondered how a diagnosis of prediabetes can escalate into type 2 diabetes?
It is not just about blood sugar levels creeping up; it is a complex journey involving insulin resistance, lifestyle factors, and even genetics.
In this article, we’ll walk through the transformation of prediabetes into type 2 diabetes, explore the contributing factors, and discuss what you can do to prevent this progression.
Article Index:
- What is Prediabetes?
- The Role of Insulin Resistance
- Lifestyle Factors and Their Impact
- How Genetics and Family History Play a Role
- Real-Life Examples: The Journey from Prediabetes to Diabetes
- Conclusion: Steps to Reverse or Manage Prediabetes
What is Prediabetes? A Silent Wake-Up Call for Your Health
Prediabetes is the body’s early distress signal that something’s off with your blood sugar regulation.
It means your blood sugar levels are higher than normal but not quite high enough to be called type 2 diabetes.
Despite how serious it sounds, prediabetes often slips under the radar—mainly because it rarely shows symptoms.
In fact, over 80% of people who have it don’t even know they do. But here’s the catch: ignoring it today could pave the way for full-blown diabetes tomorrow.
Let’s break it down point-by-point:
- It’s More Common Than You Think: According to the CDC, 96 million adults in the U.S. (roughly 1 in 3) have prediabetes. It’s not just a personal issue—it’s a public health crisis.
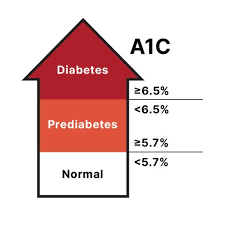
- It’s Diagnosed Through Simple Tests:
- A1C test: A result between 5.7% and 6.4% flags prediabetes.
- Fasting Plasma Glucose: Between 100–125 mg/dL indicates risk.
- Oral Glucose Tolerance Test: A 2-hour value between 140–199 mg/dL is another red flag.
- Risk Factors Abound: Being overweight, sedentary, over 45, or having a family history of diabetes increases your chances. Certain ethnic groups—like South Asians, African Americans, and Hispanics—are also more prone.
- You Can Have Prediabetes and Still Feel Fine: That’s what makes it dangerous. Most people don’t feel sick or different—until complications start to develop.
- It’s Not a Life Sentence—It’s a Chance: Lifestyle changes like losing 5–7% of your body weight and exercising 150 minutes per week can reverse prediabetes. For instance, walking briskly for 30 minutes a day can significantly lower your blood sugar over time.
- Real-Life Example: Jane, 42, discovered her A1C was 6.2% during a routine checkup. She cut back on refined carbs, started biking daily, and brought her levels back to normal in just 6 months.
Think of prediabetes not as a diagnosis, but as a fork in the road—a chance to take control before things get worse.
The Role of Insulin Resistance
To understand how prediabetes evolves into type 2 diabetes, we need to dive into the concept of insulin resistance.
In a healthy body, insulin—a hormone produced by the pancreas—helps cells absorb glucose from the bloodstream for energy.
In prediabetes, however, the cells start to resist insulin’s effects, making it harder for glucose to enter the cells.
In response, the pancreas produces more insulin to compensate and keep blood sugar levels in check.
Over time, this compensatory mechanism becomes ineffective, and blood glucose levels rise further.
Research by the National Institute of Diabetes and Digestive and Kidney Diseases highlights that insulin resistance is a key driver of both prediabetes and type 2 diabetes.
Factors such as excess abdominal fat, physical inactivity, and certain hormonal imbalances significantly contribute to developing insulin resistance.
When left unmanaged, this resistance exhausts the pancreas’s ability to produce insulin, and prediabetes transitions into type 2 diabetes.
Lifestyle Factors and Their Impact
Let us be honest—our lifestyles play a huge role in this progression.
Poor dietary choices, physical inactivity, and stress are major contributors to insulin resistance and prediabetes.
Diets high in processed foods, sugars, and unhealthy fats overload the body with glucose, putting the pancreas into overdrive.
At the same time, a sedentary lifestyle reduces the muscles’ ability to utilize glucose effectively, which worsens insulin resistance.
A study published in the Journal of Clinical Endocrinology & Metabolism shows that regular physical activity can significantly reduce the risk of developing type 2 diabetes in individuals with prediabetes.
Exercise helps the muscles become more sensitive to insulin, which aids in glucose absorption and maintains stable blood sugar levels.
On the flip side, inactivity worsens insulin resistance, making it harder for the body to control blood sugar levels effectively.
Take Tom, a 45-year-old office worker who was diagnosed with prediabetes.
His doctor pointed out that his diet of fast food and lack of physical activity were significant factors.
Tom’s doctor warned him that without changes to his lifestyle, he was on a fast track to type 2 diabetes.
It is a common story—lifestyle choices are often the tipping point between prediabetes and type 2 diabetes.
How Genetics and Family History Play a Role?
When it comes to prediabetes, your DNA might be doing more work behind the scenes than you realize.
Even if you are eating reasonably well and staying moderately active (such as swimming regularly to treat type 2 diabetes), your genetic blueprint can silently influence how your body handles glucose.
Genetics does not guarantee you would develop prediabetes—but it does load the dice.
Here’s how it breaks down, point by point:
- Family Ties Matter: If one or both of your parents have type 2 diabetes, your risk of developing prediabetes is up to 40%, and even higher if multiple relatives are affected. Siblings with diabetes? Your chances spike again. It is not just shared habits—it is also shared genes.
- Scientific Backing: Studies in Diabetes Care and The Journal of Clinical Endocrinology & Metabolism have shown that individuals with a family history of type 2 diabetes are more likely to experience early β-cell dysfunction and insulin resistance—even before blood sugar levels cross into the danger zone.
- Genetic Markers Identified: Over 80 genetic variants have been associated with type 2 diabetes and prediabetes risk. Notably, mutations in genes like TCF7L2, PPARG, and FTO impact insulin production, fat metabolism, and glucose processing.
- Ethnic Predispositions: Research from the National Institutes of Health reveals that African Americans, Native Americans, Hispanics, and South Asians have a significantly higher prevalence of insulin resistance, even at lower BMIs. This suggests that ethnicity increases type 2 diabetes risk beyond lifestyle.
- Case in Point: Maria, a Hispanic woman in her 30s, wasn’t overweight but led a sedentary life. During a routine checkup, her A1C was flagged at 6.1%. With both parents diagnosed with type 2 diabetes, her doctor emphasized the urgency of preventive action. Maria took it seriously, joined a local walking group, and added fiber-rich foods to her meals—slowing down her genetic freight train.
In short, your genes may be the blueprint, but your lifestyle is the architect. Knowing your family history can empower you to act early—and wisely.
Real-Life Examples: The Journey from Prediabetes to Diabetes
Understanding real-life cases helps illustrate how prediabetes progresses.
Research from the CDC’s National Diabetes Prevention Program (NDPP) indicates that without lifestyle changes, up to 70% of people with prediabetes will develop type 2 diabetes within five years.
For many, this progression begins subtly, as there are often no symptoms until blood sugar levels are high enough to cause noticeable issues like frequent urination, increased thirst, or fatigue.
Jack, a 50-year-old man, was diagnosed with prediabetes five years ago.
Initially, he ignored the diagnosis, thinking it wasn’t serious because he felt fine.
Over time, he started experiencing fatigue and increased thirst—classic symptoms indicating his condition was progressing to type 2 diabetes.
His story is a reminder that even without obvious symptoms, prediabetes is a serious condition that requires attention.
FAQ Section: How Prediabetes Develops into Type 2 Diabetes
Q-1: How does prediabetes develop into Type 2 Diabetes in adults in the USA?
A-1: In the United States, over 38% of adults have prediabetes, and without intervention, about 70% may eventually develop Type 2 Diabetes. The transition occurs when insulin resistance worsens and the pancreas can no longer produce enough insulin to maintain normal blood sugar levels, leading to chronic hyperglycemia.
Q-2: What are the early signs that prediabetes is turning into Type 2 Diabetes?
A-2: Early signs include increased thirst, frequent urination, fatigue, and blurred vision. However, nearly 80% of people with prediabetes are unaware of their condition, making progression difficult to detect. Blood sugar levels gradually rise beyond the prediabetes range, signaling the onset of Type 2 Diabetes.
Q-3: How fast does prediabetes progress to Type 2 Diabetes—what is the timeline?
A-3: Prediabetes can progress to Type 2 Diabetes within 3 to 5 years if no lifestyle changes are made. Studies show that about 5–10% of individuals with prediabetes convert each year, depending on risk factors such as weight, age, and activity levels.
Q-4: What risk factors cause prediabetes to become Type 2 Diabetes?
A-4: Major risk factors include obesity, physical inactivity, poor diet, and family history. Individuals with a body mass index above normal have up to a 3 times higher risk of progression. Age above 45 and abdominal fat further increase the likelihood of developing Type 2 Diabetes.
Q-5: Can prediabetes always turn into Type 2 Diabetes if left untreated?
A-5: No, prediabetes does not always lead to Type 2 Diabetes, but the risk is high. Without intervention, up to 70% of cases may progress, while the remaining may stay stable or occasionally revert to normal glucose levels. Early action plays a critical role in prevention.
Q-6: How does insulin resistance worsen from prediabetes to Type 2 Diabetes?
A-6: Insulin resistance increases as cells become less responsive to insulin. During prediabetes, the pancreas compensates by producing more insulin, but over time, this compensatory mechanism fails. This leads to a decline in insulin production by up to 50% or more, resulting in persistent high blood sugar.
Q-7: Which lifestyle habits accelerate prediabetes progression to Type 2 Diabetes?
A-7: Sedentary lifestyle, high intake of processed foods, and poor sleep patterns accelerate progression. Lack of physical activity alone can increase diabetes risk by 30–40%, while diets high in sugar and refined carbohydrates contribute significantly to worsening insulin resistance.
Q-8: How can you stop prediabetes from developing into Type 2 Diabetes naturally?
A-8: Lifestyle changes are highly effective. Losing 5–10% of body weight can reduce diabetes risk by 58%, especially when combined with at least 150 minutes of weekly physical activity. Balanced diets and regular monitoring further improve outcomes.
Q-9: What blood sugar levels indicate progression from prediabetes to Type 2 Diabetes?
A-9: Prediabetes is defined by fasting glucose levels of 100–125 mg/dL, while Type 2 Diabetes is diagnosed at 126 mg/dL or higher. HbA1c levels rising from 5.7–6.4% to 6.5% or above also indicate progression to diabetes.
Q-10: What are the long-term complications when prediabetes becomes Type 2 Diabetes?
A-10: If untreated, Type 2 Diabetes can lead to serious complications such as heart disease, kidney damage, and nerve disorders. Individuals with diabetes have a 2–4 times higher risk of cardiovascular disease, making early prevention and control essential for long-term health.
Steps to Reverse or Manage Prediabetes
The good news?
Prediabetes does not have to become type 2 diabetes.
Did you know prediabetes is reversible with lifestyle changes???
Research published in the New England Journal of Medicine and recommendations from the American Diabetes Association highlight that weight loss, increased physical activity (such as cycling to reduce A1c levels), and dietary changes can reverse prediabetes.
Here is what you can do:
Exercise Regularly: Aim for at least 150 minutes of moderate-intensity physical activity per week. Exercise improves insulin sensitivity, helping your muscles absorb glucose effectively.
Adopt a Balanced Diet: Focus on whole grains, lean proteins, and vegetables while avoiding sugary drinks and processed foods that spike blood glucose levels. Eating a diet freefrom gluten can also help stabilize blood sugar levels and reduce insulin resistance.
Monitor Your Health: Regularly check your blood glucose levels and track your A1C levels with your doctor’s guidance. Early detection and monitoring are crucial to preventing the progression from prediabetes to type 2 diabetes.
Prediabetes is a critical warning, but it does not have to define your health journey.
By making informed lifestyle changes, such as eating a balanced diet, staying active, using natural supplement for diabetes control and monitoring your health closely, you can not only manage but potentially reverse the condition.
Take action now—your future self will thank you!
References: