Obesity and Type 2 Diabetes: The Hidden Link You Can’t Ignore
- admin
- September 5, 2024
- 5:25 pm
- No Comments
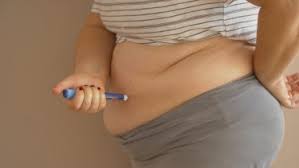
In today’s world, obesity and type 2 diabetes have become two of the most prevalent and closely linked health issues.
According to bestdietarysupplementfordiabetics.com, “It is almost impossible to talk about one without bringing up the other, but why is that?”
What makes these two conditions so interconnected? And, more importantly, how can we break this vicious cycle?
In this article, I will explore:
- The relationship between obesity and type 2 diabetes.
- The biological mechanisms that link the two conditions.
- How obesity contributes to insulin resistance.
- Actionable steps to prevent or reverse the damage.
- FAQs on Obesity & Type 2 Diabetes
- Science-backed strategies to manage both conditions effectively.
By the end, you will have a deeper understanding of why obesity and type 2 diabetes are so tightly connected and how you can take control of your health.
What is Type 2 Diabetes and How Does It Relate to Obesity?
Type 2 diabetes is a chronic condition where your body either does not produce enough insulin or becomes resistant to insulin, the hormone responsible for regulating blood sugar levels.
Without sufficient insulin, glucose builds up in the bloodstream, leading to high blood sugar levels, which can damage vital organs over time.
Obesity, on the other hand, refers to having excess body fat, typically due to an imbalance between calorie intake and energy expenditure. But here is where the connection comes in: over 85% of people with type 2 diabetes are overweight or obese.
Being obese increases the body’s demand for insulin because excess fat interferes with how insulin functions, leading to insulin resistance, which is the hallmark of type 2 diabetes.
The key takeaway? Obesity doesn’t just increase the likelihood of developing type 2 diabetes—it often accelerates its progression and worsens its impact.

The Science Behind the Link: Insulin Resistance and Fat Cells
So, how exactly does obesity cause type 2 diabetes?
It all comes down to insulin resistance and the role that fat cells (also known as adipocytes) play in our metabolism.
Insulin Resistance:
Normally, insulin allows glucose to enter cells where it is used for energy.
But when someone is obese, particularly with excess fat around the abdomen (known as visceral fat), the fat cells become inflamed and disrupt this process.
This leads to insulin resistance, meaning that your cells become less responsive to insulin, forcing the pancreas to work overtime to produce more of it.
Over time, the pancreas cannot keep up, and blood sugar levels begin to rise.
Chronic Inflammation:
Obesity is associated with low-grade, chronic inflammation. Fat cells, especially those in visceral fat, release insulin disrupting inflammatory substances called cytokines.
These cytokines interfere with insulin signaling pathways, making it harder for insulin to do its job.
This inflammatory response not only worsens insulin resistance but also increases the risk of heart disease and other complications that often accompany type 2 diabetes.
Fat Distribution Matters:
Not all fat is created equal.
People with more visceral fat—fat stored around internal organs—are at a much higher risk of developing insulin resistance compared to those with subcutaneous fat (the fat stored under the skin).
Research has shown that even if two people have the same body mass index (BMI), the one with more visceral fat is more likely to develop type 2 diabetes.
The Role of Diet and Lifestyle
While genetics do play a role in obesity and type 2 diabetes, diet and lifestyle choices are often the primary drivers.
Here is why:
High-Calorie Diets:
Consuming more calories than your body needs, especially from processed foods high in sugars and unhealthy fats, leads to weight gain.
Foods high in refined carbs and sugars such as hot dogs cause blood sugar spikes, forcing the pancreas to produce more insulin.
Over time, this can lead to insulin resistance and type 2 diabetes.
Sedentary Lifestyle:
Physical inactivity is another major factor. When you don’t exercise regularly, your body uses less glucose for energy, leading to higher blood sugar levels.
Exercise also improves insulin sensitivity, meaning your body can use insulin more efficiently. Regular physical activity can significantly reduce the risk of both obesity and type 2 diabetes.
Stress and Sleep:
Chronic stress and poor sleep are often overlooked contributors.
Stress hormones, such as cortisol, raise blood sugar levels, while sleep deprivation has been linked to insulin resistance.
Both factors can drive weight gain and make it harder to manage blood sugar levels.
Prevention and Reversal: Breaking the Cycle
The connection between obesity and type 2 diabetes might seem daunting, but there is good news: both conditions are largely preventable and, in some cases, reversible through lifestyle changes. Let’s look at the steps you can take to break the cycle.
Weight Loss
Losing weight, even just 5-10% of your body weight, can significantly improve insulin sensitivity and lower your risk of developing type 2 diabetes. A study published in The Lancet found that individuals who lost weight through diet and exercise were able to reverse type 2 diabetes symptoms and, in some cases, achieve remission.
Healthy Diet
Adopting a balanced low glycemic diet rich in whole foods, fiber, lean proteins, and healthy fats can make a massive difference in controlling both weight and blood sugar levels.
Focus on:
- Complex carbohydrates like whole grains, vegetables, and legumes, which break down more slowly and prevent blood sugar spikes.
- Healthy fats like those found in avocados, nuts, and olive oil, which support insulin function.
- High-fiber foods that help keep you full and improve blood sugar control.
Exercise
Regular physical activity, such as walking, swimming, or strength training, can dramatically improve insulin sensitivity and aid in weight management. Aim for at least 150 minutes of moderate-intensity exercise per week. Studies show that combining aerobic exercise with resistance training is especially effective at controlling blood sugar and reducing visceral fat.
Mindful Eating and Portion Control
Being mindful of what you eat and how much can prevent overeating, which is a significant contributor to obesity.
By slowing down and focusing on portion control, you can better manage calorie intake and avoid the binge-eating cycles that often lead to weight gain.
FAQs on Obesity & Type 2 Diabetes
Q-1: How does obesity lead to Type 2 Diabetes in adults in the USA?
A-1: In the United States, over 42% of adults are obese, and studies show that obesity accounts for nearly 80–85% of Type 2 Diabetes cases. Excess fat, especially abdominal fat, triggers insulin resistance, where cells stop responding effectively to insulin. This leads to elevated blood sugar levels over time. Research confirms that obese adults are 5–7 times more likely to develop Type 2 Diabetes than those with a healthy weight.
Q-2: What is the link between insulin resistance, obesity, and Type 2 Diabetes?
A-2: Insulin resistance is the critical bridge connecting obesity to diabetes. Around 70% of obese individuals develop some degree of insulin resistance. Fat cells release inflammatory chemicals that impair insulin function. Over time, the pancreas struggles to keep up, leading to Type 2 Diabetes. This progression has been widely observed in long-term population studies.
Q-3: Can losing weight reverse Type 2 Diabetes naturally?
A-3: Yes, weight loss can significantly improve or even reverse Type 2 Diabetes in many cases. Studies show that 46% of individuals achieved remission after losing around 10–15% of body weight. Additionally, losing just 5–10% of body weight reduces diabetes risk by 58%, making weight management a powerful tool in prevention and control.
Q-4: What is the best diet for managing obesity and Type 2 Diabetes in 2026?
A-4: Diets focusing on whole foods and low glycemic load are highly effective. Mediterranean-style diets reduce diabetes risk by 30%, while high-fiber diets improve blood sugar control by 20–30%. Reducing processed food intake also significantly lowers obesity-related complications and supports long-term metabolic health.
Q-5: What role does visceral fat play in Type 2 Diabetes risk?
A-5: Visceral fat, stored around internal organs, is more harmful than subcutaneous fat. Individuals with high visceral fat have a 2–3 times higher risk of developing Type 2 Diabetes. Central obesity is considered a stronger predictor of diabetes risk than overall body weight.
Q-6: How do GLP-1 weight loss drugs impact Type 2 Diabetes outcomes?
A-6: GLP-1 receptor agonists have significantly improved treatment outcomes. Clinical trials show these medications can reduce body weight by 15–20% and lower HbA1c levels by 1.5–2%. They also help improve blood sugar control and reduce cardiovascular risks in individuals with Type 2 Diabetes.
Q-7: What are the early signs of obesity-related Type 2 Diabetes symptoms in adults?
A-7: Early symptoms include fatigue, frequent urination, and increased thirst. However, nearly 50% of adults remain undiagnosed in the early stages. Early detection can improve management outcomes by over 60%, making regular screening important, especially for obese individuals.
Q-8: How can overweight or obese individuals prevent Type 2 Diabetes?
A-8: Prevention is highly achievable through lifestyle changes. Structured programs show a 58% reduction in diabetes risk, and up to 71% reduction in adults over 60. Regular exercise (at least 150 minutes per week) and modest weight loss are key strategies for prevention.
Q-9: BMI vs waist circumference—what matters more for diabetes risk?
A-9: While BMI is commonly used, waist circumference is a better predictor of diabetes risk. Abdominal obesity can increase risk by up to 70%, even in individuals with a normal BMI. Combining both measurements provides a more accurate assessment of risk.
Q-10: What lifestyle changes help reduce obesity and control blood sugar levels?
A-10: Sustainable lifestyle changes can significantly improve health outcomes. Regular physical activity lowers diabetes risk by 30–40%, while balanced diets improve blood sugar control by 25% or more. Consistency, stress management, and adequate sleep further enhance long-term metabolic health.

The Solution to Obesity and Type 2 Diabetes
The link between obesity and type 2 diabetes is undeniable, but the good news is that both conditions are largely preventable and manageable.
By addressing the root causes—such as poor diet, lack of exercise, and chronic stress—you can break the cycle of insulin resistance and regain control over your health.
What You can Do?
If you are at risk for type 2 diabetes or already dealing with the condition, the best course of action is to focus on sustainable lifestyle changes.
I make it a point to include supplements that Lower Blood Sugar Fast into my Type 2 Diabetic diet routine.
Small, consistent efforts toward weight loss, healthy eating, and regular exercise can make a significant difference.
Additionally, seeking support from healthcare professionals, dietitians, and even diabetes support groups can provide guidance and motivation along the way.
Remember, you have the power to reverse the trajectory of your health.
Start today, and watch as the positive changes ripple through your life.
References: