How Enterovirus Causes Type 1 Diabetes?
- admin
- March 12, 2026
- 6:25 am
- No Comments
Type 1 diabetes is an autoimmune condition in which the body’s immune system mistakenly destroys the insulin-producing beta cells located in the pancreas.
Insulin is a vital hormone that helps glucose move from the bloodstream into cells for energy. When these cells are destroyed, the body cannot produce enough insulin, causing blood sugar levels to rise abnormally.
Unlike Type 2 diabetes, which is often influenced by lifestyle and metabolic factors, Type 1 diabetes usually develops due to a combination of genetic predisposition and environmental triggers.
Over the past two decades, researchers have identified viral infections as one of the most important environmental triggers.
Among these viruses, enteroviruses have been studied extensively for their possible role in initiating the autoimmune process.
Enteroviruses are extremely common viruses that infect millions of people every year. Most infections occur during childhood and typically cause mild symptoms such as fever, sore throat, diarrhea, or skin rash.
However, scientific studies suggest that in genetically susceptible individuals, certain strains of enteroviruses may trigger immune reactions that lead to the destruction of pancreatic beta cells.
Epidemiological research indicates that children exposed to enterovirus infections may have about 40–50% higher risk of developing Type 1 diabetes compared to children who are not infected.
In addition, some studies have found that individuals with Type 1 diabetes are up to eight to ten times more likely to show evidence of previous enterovirus infection.
These findings have strengthened the scientific hypothesis that viral infections may initiate or accelerate the autoimmune process responsible for Type 1 diabetes.
Understanding how enteroviruses affect the immune system and pancreatic cells is crucial for developing preventive strategies such as vaccines, early screening methods, and targeted therapies.
This article by bestdietarysupplementfordiabetics.com explains the biological mechanisms through which enteroviruses may contribute to the development of Type 1 diabetes.
Article Index
- Understanding Enteroviruses
- Global Statistics of Type 1 Diabetes
- The Role of Genetics in Type 1 Diabetes
- How Enteroviruses Infect the Human Body
- Viral Infection of Pancreatic Beta Cells
- Immune System Activation and Autoimmune Damage
- Molecular Mimicry and Immune Confusion
- Persistent Viral Infection in the Pancreas
- Childhood Exposure and Environmental Risk Factors
- Why Enterovirus Infection Does Not Cause Diabetes in Everyone
- Frequently Asked Questions (Top Long-Tail Keywords)
- Conclusion
Understanding Enteroviruses
Enteroviruses are a group of viruses belonging to the Picornaviridae family. Scientists have identified more than 100 different enterovirus types capable of infecting humans. Some of the most well-known members of this group include polioviruses, echoviruses, and coxsackieviruses.
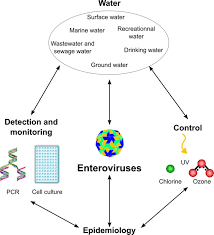
These viruses spread mainly through contaminated food, water, respiratory droplets, and close contact with infected individuals. Because they spread easily, enteroviruses are extremely common, particularly among children.
Most infections occur before the age of five, and the majority of people are exposed to several enterovirus strains during childhood. While many infections cause mild illnesses such as fever, cough, stomach upset, or rash, certain strains have the ability to infect internal organs including the heart, nervous system, and pancreas.
One strain that has drawn particular attention in diabetes research is Coxsackievirus B. Laboratory studies show that this virus can infect pancreatic beta cells, which are responsible for producing insulin. When these cells are infected, they may become damaged or may trigger an abnormal immune response.
Because enteroviruses are widespread and frequently infect children, researchers have been investigating whether repeated exposure to these viruses may play a role in initiating autoimmune diseases such as Type 1 diabetes.
Global Statistics of Type 1 Diabetes
Type 1 diabetes represents approximately 5–10% of all diabetes cases worldwide. Although it is less common than Type 2 diabetes, the condition has been steadily increasing in many countries.
Globally, more than 8.7 million people live with Type 1 diabetes, and the disease is most often diagnosed during childhood or adolescence. In the United States alone, around 1.6 million individuals currently live with the condition.
One of the most concerning trends is that the incidence of Type 1 diabetes has been increasing by about 3–4% per year globally. Scientists believe this rapid increase cannot be explained by genetics alone because human genetic patterns change very slowly over generations.
This observation has led researchers to investigate environmental factors that may trigger autoimmune destruction of pancreatic cells. Viral infections are among the most strongly suspected triggers.
Large population studies analyzing hundreds of thousands of children have shown that viral infections often occur before the appearance of diabetes-related autoantibodies, which are early markers of autoimmune damage. This timing suggests that infections may initiate the immune reaction that eventually leads to Type 1 diabetes.
The Role of Genetics in Type 1 Diabetes
Although viral infections may trigger the disease, genetics plays a crucial role in determining who develops Type 1 diabetes.
Certain immune system genes increase the likelihood that the body will respond abnormally to infections. Individuals carrying these genes have a higher risk of developing autoimmune diseases, including Type 1 diabetes.
Research shows that people with a family history of Type 1 diabetes have up to 15 times greater risk of developing the condition compared with the general population. However, genetics alone does not determine the outcome.
Many individuals who carry high-risk genes never develop Type 1 diabetes, which indicates that environmental triggers are necessary to activate the autoimmune process. Viral infections such as enteroviruses are believed to be one of the most important triggers in genetically susceptible individuals.
When a person with genetic susceptibility encounters certain viruses, the immune system may respond in a way that damages the body’s own tissues. In the case of Type 1 diabetes, the target becomes the insulin-producing beta cells in the pancreas.
How Enteroviruses Infect the Human Body?
Enteroviruses typically enter the body through the digestive system or respiratory tract. After entering the body, the virus begins multiplying in the throat, intestines, or nearby lymph nodes.
Within a few days, the virus may enter the bloodstream and spread to other organs. This phase of infection is known as viremia.
Once in the bloodstream, enteroviruses can reach different tissues including muscles, nerves, heart tissue, and in some cases the pancreas. The virus attaches to specific receptors on the surface of cells and enters the cell.
After entering the cell, the virus uses the cell’s machinery to replicate itself. This process produces thousands of new viral particles that can infect neighboring cells.
In many individuals, the immune system quickly eliminates the virus before significant damage occurs. However, if the virus infects pancreatic cells or triggers abnormal immune reactions, the infection may contribute to autoimmune damage that leads to Type 1 diabetes.
Viral Infection of Pancreatic Beta Cells
The pancreas contains clusters of cells known as the islets of Langerhans, which produce hormones that regulate blood sugar. Within these islets are beta cells that produce insulin.
Some enteroviruses have the ability to infect these beta cells directly. Laboratory studies have demonstrated that Coxsackievirus B can enter beta cells and replicate inside them.
When the virus infects these cells, several harmful effects may occur:
- The infected cells may become damaged or die
• Viral proteins may appear on the surface of the cells
• The immune system may identify infected cells as abnormal
As immune cells attempt to eliminate the infection, they may begin attacking the infected beta cells. Unfortunately, this immune attack can sometimes continue even after the virus has disappeared.
Gradually, the immune system destroys increasing numbers of beta cells. When around 80–90% of these cells are lost, the pancreas can no longer produce enough insulin to regulate blood glucose levels.
At this stage, symptoms of Type 1 diabetes begin to appear.
Immune System Activation and Autoimmune Damage
The immune system normally protects the body from harmful pathogens such as bacteria and viruses. When a virus enters the body, immune cells release signaling molecules that activate defensive responses.
However, in some cases, viral infections can disrupt normal immune regulation. Instead of attacking only infected cells, the immune system may begin attacking healthy tissues.
This abnormal reaction is known as autoimmunity.
In individuals who later develop Type 1 diabetes, immune cells produce antibodies that specifically target proteins found in pancreatic beta cells. These antibodies can often be detected years before the actual diagnosis of diabetes.
The immune system gradually destroys beta cells over time. Once the majority of beta cells are destroyed, insulin production drops sharply, leading to elevated blood sugar levels and the symptoms of Type 1 diabetes.
Molecular Mimicry and Immune Confusion
One explanation for how viruses trigger autoimmune diseases is a phenomenon called molecular mimicry.
Molecular mimicry occurs when viral proteins resemble proteins naturally present in human tissues. Because of this similarity, the immune system may become confused and attack both the virus and the body’s own cells.
In the case of enteroviruses, some viral proteins resemble proteins found in pancreatic beta cells. When the immune system produces antibodies to attack the virus, these antibodies may also target beta cells.
This mistaken identity can cause the immune system to continue attacking pancreatic cells even after the viral infection has ended. Over time, this immune attack leads to the progressive loss of insulin-producing cells and the development of Type 1 diabetes.
Persistent Viral Infection in the Pancreas
Another possible mechanism linking enteroviruses to Type 1 diabetes involves persistent infection.
In some individuals, the virus may remain inside pancreatic cells for long periods without causing obvious symptoms. This low-level infection may continuously stimulate the immune system.
Persistent viral presence can cause chronic inflammation within the pancreas. Chronic inflammation damages tissues and may accelerate the autoimmune destruction of beta cells.
Researchers studying pancreatic tissue samples have detected viral genetic material in individuals with Type 1 diabetes, suggesting that persistent infection may contribute to disease progression in certain cases.
Childhood Exposure and Environmental Risk Factors
Type 1 diabetes most often develops during childhood or adolescence. This timing is significant because children experience frequent viral infections during early life.
Several environmental factors may increase the likelihood that enterovirus infections trigger autoimmune responses:
- Early childhood viral exposure
• Seasonal viral outbreaks
• Crowded living environments
• Nutritional deficiencies
• Immune system immaturity
Because children’s immune systems are still developing, infections during early life may have stronger effects on immune regulation.
Scientists believe that repeated viral infections during childhood may gradually influence immune behavior, increasing the probability of autoimmune diseases in genetically susceptible individuals.
Why Enterovirus Infection Does Not Cause Diabetes in Everyone?
Despite the strong association between enteroviruses and Type 1 diabetes, most people who experience these infections never develop diabetes.
Several protective factors help prevent autoimmune disease:
- Strong immune regulation
• Absence of high-risk genetic markers
• Rapid viral clearance by the immune system
• Limited viral damage to pancreatic cells
Additionally, not all enterovirus strains are capable of infecting pancreatic cells. Many strains cause only mild respiratory or digestive infections without affecting the pancreas.
This combination of genetic protection, immune balance, and viral characteristics explains why only a small proportion of infected individuals eventually develop Type 1 diabetes.
FAQs on Entrovirus & Type 1 Diabetes
Q-1: Can enterovirus cause Type 1 diabetes?
A-1: Yes. Scientific evidence suggests that enterovirus infections may act as environmental triggers for Type 1 diabetes in genetically susceptible individuals.
Global research projects led by the Centers for Disease Control and Prevention (CDC), National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), and University of Helsinki have found that children exposed to enteroviruses may have 40–50% higher risk of developing Type 1 diabetes compared with those who are not infected.
These viruses can infect pancreatic tissue and stimulate immune responses that mistakenly attack insulin-producing beta cells.
Worldwide, Type 1 diabetes affects about 8.7 million people, including 1.6 million individuals in the United States, indicating why identifying viral triggers is an important area of medical research.
Q-2: Which virus is most linked to Type 1 diabetes?
A-2: The virus most strongly linked to Type 1 diabetes is Coxsackievirus B, part of the enterovirus family.
Studies conducted by Karolinska Institute (Sweden), Tampere University (Finland), and the National Institutes of Health (NIH) show that this virus can infect pancreatic beta cells directly. Coxsackievirus B strains, especially B1 to B6, can replicate inside these cells and trigger immune reactions.
Research from Northern Europe—where Type 1 diabetes rates are among the highest globally—shows that children infected with certain Coxsackievirus strains may have up to twice the risk of developing diabetes-related autoantibodies.
Q-3: How does a virus trigger autoimmune diabetes?
A-3: Viruses may trigger autoimmune diabetes through three main mechanisms: direct beta-cell infection, immune inflammation, and molecular mimicry.
Molecular mimicry occurs when viral proteins resemble proteins found in pancreatic cells. Studies from the Joslin Diabetes Center (Boston) and University of Cambridge show that immune cells may attack both the virus and insulin-producing cells due to this similarity.
Once the immune attack begins, beta-cell destruction may continue for years before symptoms appear.
Q-4: Can viruses destroy pancreatic beta cells?
A-4: Yes. Certain viruses can infect and damage pancreatic beta cells directly.
Research from The Scripps Research Institute and University of Colorado Anschutz Medical Campus shows that enteroviruses can replicate inside beta cells and cause cellular stress or death.
In addition, immune cells such as T-lymphocytes may attack infected cells.
By the time Type 1 diabetes is diagnosed, approximately 80–90% of beta cells are already destroyed, which explains why lifelong insulin therapy becomes necessary.
Q-5: What percentage of Type 1 diabetes is linked to viruses?
A-5: Scientists estimate that viral infections may contribute to 30–50% of new Type 1 diabetes cases, particularly in children.
Studies from Uppsala University, Baylor College of Medicine, and International Diabetes Federation data show that people with Type 1 diabetes are up to 8–10 times more likely to show evidence of prior enterovirus infection.
Globally, about 500,000 children are diagnosed each year, and incidence rates are increasing by 3–4% annually, suggesting environmental triggers such as viruses may influence this trend.
Q-6: Are children more vulnerable to viral triggers of Type 1 diabetes?
A-6: Yes. Children experience frequent infections because their immune systems are still developing.
According to CDC surveillance data, young children may experience 6–8 viral infections per year.
Large research programs such as the TEDDY Study (The Environmental Determinants of Diabetes in the Young)—conducted in the United States, Finland, Germany, and Sweden—have shown that viral infections often appear before diabetes-related autoantibodies develop.
Q-7: Can preventing viral infections reduce Type 1 diabetes risk?
A-7: Possibly. Researchers at Tampere University, University of Oxford, and the NIH Vaccine Research Center are developing vaccines targeting Coxsackievirus B.
Early studies suggest that preventing certain viral infections could potentially reduce Type 1 diabetes incidence by 10–20% in high-risk populations, though vaccines are still under investigation.
Q-8: How common are enterovirus infections?
A-8: Enterovirus infections are extremely common. According to World Health Organization (WHO) and CDC surveillance reports, 10–15 million symptomatic enterovirus infections occur annually in the United States alone. Globally, tens of millions of cases occur each year, particularly among children under five.
Q-9: Can Type 1 diabetes develop years after a viral infection?
A-9: Yes. The autoimmune process can begin long before symptoms appear. Research from Joslin Diabetes Center and University of Florida Diabetes Institute shows that diabetes-related autoantibodies may appear 5–10 years before diagnosis, while beta-cell destruction gradually progresses.
Q-10: Is Type 1 diabetes caused only by viruses?
A-10: No. Type 1 diabetes is a multifactorial disease. More than 50 genes, including specific HLA genes on chromosome 6, influence disease risk. Twin studies show that identical twins share the disease only 30–50% of the time, proving that environmental triggers such as viruses, immune responses, and lifestyle factors all contribute to the development of Type 1 diabetes.
Conclusive Analysis
Type 1 diabetes develops when the immune system destroys the insulin-producing beta cells of the pancreas.
While genetics determines susceptibility, environmental triggers often initiate the autoimmune process. Among these triggers, enteroviruses have emerged as one of the most significant candidates.
Enteroviruses are widespread viruses that infect millions of people each year, particularly children.
Scientific studies show that individuals who experience enterovirus infections may have a significantly higher likelihood of developing Type 1 diabetes compared with those who have not been infected.
These viruses may contribute to diabetes through several mechanisms.
They can directly infect pancreatic beta cells, trigger immune system activation, cause molecular mimicry that confuses immune defenses, or persist in pancreatic tissue and create chronic inflammation. Over time, these processes can lead to the gradual destruction of insulin-producing cells.
However, enterovirus infection alone does not guarantee the development of diabetes. The disease usually appears when genetic susceptibility, immune dysfunction, and environmental triggers interact together.
Understanding the connection between viral infections and autoimmune diseases is an important area of modern medical research.
Continued studies may lead to new strategies such as vaccines, antiviral therapies, and early screening programs that could help prevent or delay the onset of Type 1 diabetes in future generations.
Recommended:
- https://bestdietarysupplementfordiabetics.com/is-coxsackievirus-behind-the-surge-in-type-1-diabetes/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9242008/
- https://diabetesjournals.org/diabetes/article/61/3/687/15699/Type-1-Diabetes-Is-Associated-With-Enterovirus
- Why trust bestdietarysupplementfordiabetics.com?
- For educational purposes only