How Gallstones Trigger Pancreatic Inflammation in Type 3c Diabetes?
- admin
- November 6, 2024
- 9:12 pm
- No Comments
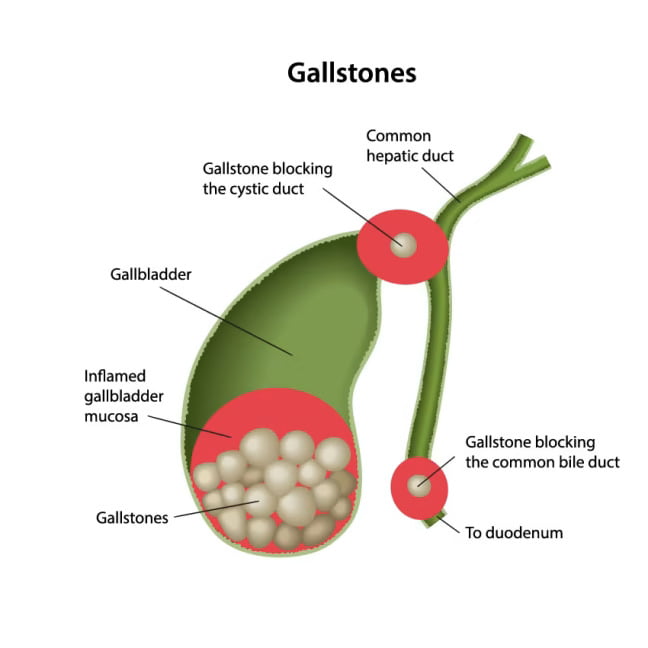
Gallstones, those tiny stones formed in the gallbladder, can unexpectedly wreak havoc on more than just digestive health.
In this article, BestDietarySupplementforDiabetics is exploring how gallstones can lead to pancreatic inflammation, sometimes resulting in Type 3c diabetes, a form of diabetes tied directly to pancreatic conditions.
What to Expect in This Article?
In this comprehensive guide, we’ll discuss:
- What gallstones are and how they form
- The connection between gallstones and pancreatic inflammation
- How inflammation caused by gallstones can damage pancreatic cells
- Why this leads to Type 3c diabetes
- FAQs on How Gallstones Lead to Inflammation in Type 3c Diabetes
- Real-life examples to illustrate how gallstones affect pancreatic health
So, let’s dive in and see how these small stones can lead to a big impact on pancreatic function and blood sugar regulation.
What Are Gallstones and How Do They Form?
Gallstones are small, hardened deposits that form in the gallbladder, typically made up of cholesterol or bilirubin.
While these stones might remain harmless for some people, they can cause significant health issues when they migrate or block bile flow.
How Gallstones Form?
When the balance of substances like cholesterol, bile salts, and bilirubin is off in the gallbladder, it can result in the formation of these stones.
Many factors influence gallstone formation, including obesity, high cholesterol diets, genetic mutations, and certain medications.
According to research in the Journal of Gastroenterology, hormonal imbalances can also increase the risk, particularly in women.
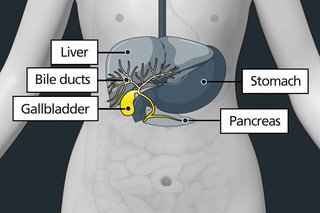
The Gallbladder and Pancreas: A Complicated Relationship
Though separate organs, the gallbladder and pancreas share a common pathway.
When bile or pancreatic fluid cannot flow freely, it can back up and lead to inflammation.
This close anatomical relationship means that issues in the gallbladder often directly impact the pancreas.
Example:
Consider Emily, a 52-year-old who developed gallstones after years of high-cholesterol diets and infrequent exercise.
One gallstone eventually blocked her bile duct, leading to an unexpected inflammation of her pancreas—a condition called pancreatitis.
Emily’s doctors explained that her pancreas was under stress, making it harder to produce insulin.
Key Insight:
Pancreatitis, often linked with gallstone obstruction, can lead to Type 3c diabetes, which differs from Type 1 and Type 2 diabetes as it is triggered by pancreatic damage.
How Gallstones Lead to Pancreatic Inflammation?
Gallstones can obstruct the pancreatic duct, leading to what is known as “biliary pancreatitis.”
This blockage stops pancreatic enzymes from flowing normally, and as a result, these enzymes begin to digest pancreatic tissue, causing inflammation.
Scientific Perspective on Biliary Pancreatitis
Studies such as those in the American Journal of Gastroenterology reveal that gallstones can initiate pancreatic damage by blocking the main pancreatic duct.
The duct blockage increases the pressure, leading to the release of digestive enzymes within the pancreas itself—essentially causing the pancreas to “digest” its own tissue.
Hormonal Impact:
This inflammation can trigger hormone disruptions within the pancreas, especially affecting insulin production, which we will discuss shortly.
How Pancreatic Inflammation Affects Insulin Production?
When gallstones trigger pancreatic inflammation, the pancreas’ ability to produce insulin is compromised.
Insulin, a hormone essential for regulating blood sugar, is produced by specialized cells in the pancreas.
Inflammation can disrupt or even destroy these cells, affecting blood sugar control.
According to a study published in Endocrine Reviews, chronic pancreatitis frequently leads to “Type 3c diabetes,” a diabetes subtype directly associated with pancreatic injury.
Here is how:
- Damage to Beta Cells: Inflammation from pancreatitis impairs insulin-producing beta cells, reducing insulin production.
- Scarring and Fibrosis: Chronic inflammation leads to fibrosis or scarring, permanently damaging pancreatic tissue.
- Hormone Imbalance: Inflammation also disrupts other pancreatic hormones, such as glucagon, making blood sugar regulation even harder.
Real-Life Example:
James, a 45-year-old accountant, struggled with recurring pancreatitis due to gallstones.
After multiple episodes, his doctor noted that James’ blood sugar levels were erratic—a clear indication that his pancreatic function was compromised.
Soon after, James was diagnosed with Type 3c diabetes, a condition rooted in his damaged pancreatic tissue.
So, he took the help of the best supplements to lower blood sugar. Luckily for James, they got the job done by stabilizing his fluctuating blood sugar levels.
Type 3c Diabetes: What Makes It Different?
Type 3c diabetes, also known as pancreatogenic diabetes, is a unique form of diabetes directly related to pancreatic disease.
Unlike Type 1 or Type 2 diabetes, Type 3c stems from pancreatic injury, often through inflammation or removal of part of the pancreas.
Key characteristics include:
- Insulin Deficiency and Glucose Intolerance: Since the pancreas is damaged, insulin production is lower, leading to higher blood sugar levels.
- Digestive Enzyme Insufficiency: Patients may experience digestive issues since the pancreas also helps digest food.
- Tied to Pancreatic Diseases: Studies show that people with pancreatitis or pancreatic injury, like that caused by gallstones, have a higher chance of developing Type 3c diabetes (Diabetes Care journal).
Why Gallstones Increase Risk for Type 3c Diabetes?
With gallstones frequently causing pancreatitis, people with gallstone issues are at a higher risk for Type 3c diabetes.
The inflammation caused by these stones leads to repeated injury to the pancreas, eventually resulting in reduced insulin-producing cells and digestive function.
Signs and Symptoms of Gallstone-Induced Pancreatic Inflammation
Recognizing the symptoms of pancreatic inflammation triggered by gallstones is essential for early intervention.
Common symptoms include:
- Abdominal Pain: Often severe and radiating to the back.
- Jaundice: Yellowing of the skin, indicating bile duct obstruction.
- Nausea and Vomiting: Common symptoms of both pancreatitis and gallstone obstruction.
- Blood Sugar Changes: High blood sugar levels or erratic blood sugar patterns, indicating a compromised pancreas.
Case Study:
Sarah, a 38-year-old mother of two, noticed a pattern of severe abdominal pain after eating fatty meals.
When she developed jaundice, she visited her doctor, who diagnosed her with gallstone-related pancreatitis.
Later, Sarah was informed that the inflammation had damaged her pancreas’ ability to produce insulin, resulting in Type 3c diabetes.
Long-Term Effects of Gallstone-Induced Pancreatic Inflammation
The long-term effects of pancreatic inflammation due to gallstones can be significant, impacting not only blood sugar but overall health:
- Increased Risk of Diabetes: Persistent inflammation damages pancreatic cells, heightening the risk for Type 3c diabetes.
- Chronic Pancreatitis: Recurrent gallstone obstructions can lead to chronic pancreatitis, a condition that is both painful and difficult to manage.
- Digestive Complications: Pancreatic enzymes are essential for digestion; without them, patients may experience malnutrition or weight loss.
Research Insight:
According to Gastroenterology and Hepatology research, chronic pancreatitis, often stemming from gallstones, not only leads to digestive issues but is a significant contributor to diabetes, particularly Type 3c diabetes.
FAQs on How Pancreatic Inflammation is Caused by Gallstones in Type 3c Diabetes:
Q-1: How do gallstones cause pancreatitis leading to Type 3c diabetes?
A-1: Gallstones can migrate from the gallbladder into the bile duct and block the pancreatic duct. This blockage traps digestive enzymes inside the pancreas, causing inflammation known as pancreatitis.
Over time, repeated inflammation damages insulin-producing cells, leading to Type 3c diabetes (pancreatogenic diabetes). In the U.S., gallstones account for nearly 40–50% of acute pancreatitis cases, according to the National Institutes of Health.
Q-2: What is the mechanism of gallstone blockage in the pancreatic duct?
A-2: The bile duct and pancreatic duct share a common opening into the small intestine. When a gallstone lodges at this junction, it blocks the flow of both bile and pancreatic enzymes. This leads to enzyme buildup, causing the pancreas to “digest itself,” triggering inflammation and tissue injury.
Q-3: What is the link between gallstone pancreatitis and pancreatogenic diabetes?
A-3: Recurrent gallstone-induced pancreatitis can destroy both the exocrine (digestive) and endocrine (hormonal) functions of the pancreas. This dual damage leads to Type 3c diabetes, which differs from Type 1 and Type 2. The Cleveland Clinic notes that chronic pancreatitis is a leading cause of this condition.
Q-4: Can gallstones permanently damage the pancreas and cause insulin deficiency?
A-4: Yes. Severe or repeated inflammation can scar pancreatic tissue, reducing its ability to produce insulin. This results in unstable blood sugar levels and eventual diabetes. Studies show that up to 30% of chronic pancreatitis patients develop diabetes.
Q-5: How does bile duct obstruction increase diabetes risk?
A-5: Bile duct obstruction leads to prolonged pancreatic inflammation. Chronic inflammation damages beta cells, which are responsible for insulin production. Without sufficient insulin, glucose regulation becomes impaired, increasing diabetes risk.
Q-6: What role does recurrent gallstone pancreatitis play in Type 3c diabetes?
A-6: Each episode of pancreatitis adds cumulative damage. Over time, repeated attacks reduce pancreatic function significantly. Clinical data suggest that recurrent pancreatitis increases the likelihood of diabetes by 2–3 times compared to a single episode.
Q-7: How do gallstones affect long-term pancreatic function?
A-7: Long-term effects include reduced enzyme production, poor digestion, and impaired insulin secretion. Patients may experience both malnutrition and blood sugar imbalances. The American Gastroenterological Association highlights that chronic pancreatic damage can lead to lifelong metabolic complications.
Q-8: What is the scientific explanation behind gallstone-induced pancreatic inflammation?
A-8: When enzymes like trypsin are prematurely activated inside the pancreas due to duct blockage, they begin breaking down pancreatic tissue. This triggers an inflammatory cascade, leading to swelling, cell death, and fibrosis over time.
Q-9: What is the risk of developing Type 3c diabetes after gallstone pancreatitis?
A-9: Research indicates that 10–20% of patients with acute pancreatitis may develop diabetes within a few years, especially if episodes are severe or recurrent. The Centers for Disease Control and Prevention emphasizes monitoring glucose levels after pancreatitis.
Q-10: How does pancreatic inflammation lead to endocrine dysfunction?
A-10: Inflammation damages the islets of Langerhans, which produce insulin and glucagon. This disrupts glucose balance, leading to unstable blood sugar levels—a hallmark of Type 3c diabetes.
Q-11: What symptoms indicate gallstone-related pancreatic damage?
A-11: Symptoms include severe abdominal pain, nausea, vomiting, unexplained weight loss, and fluctuating blood sugar levels. Early diagnosis is crucial to prevent long-term complications.
Q-12: Are certain individuals at higher risk of this condition in the U.S.?
A-12: Yes. Risk factors include obesity, high-fat diets, and sedentary lifestyles. In the U.S., over 25 million people are affected by gallstones, increasing the risk of pancreatitis and related complications.
Q-13: Can early treatment of gallstones prevent Type 3c diabetes?
A-13: Absolutely. Removing gallstones or the gallbladder (cholecystectomy) can prevent recurrent pancreatitis. Early intervention significantly reduces the risk of long-term pancreatic damage.
Q-14: What lifestyle changes can reduce the risk of gallstone-related complications?
A-14:
- Maintain a healthy weight
- Follow a balanced, low-fat diet
- Exercise regularly (150 minutes/week recommended by the Centers for Disease Control and Prevention)
- Avoid rapid weight loss
These steps help prevent gallstone formation and protect pancreatic health.
Q-15: Can pancreatic function improve after treatment?
A-15: In mild cases, pancreatic function may partially recover after inflammation subsides. However, severe or chronic damage is often irreversible. Early detection and management are key to preserving function.
Free Tip of the Day:
Gallstones may seem like a minor digestive issue, but their impact on the pancreas can be profound. By blocking critical ducts, they can trigger inflammation that progressively damages both digestive and hormonal functions of the pancreas.
In the U.S., where gallstones and metabolic disorders are common, understanding this connection is crucial. The progression from gallstones to pancreatitis and eventually Type 3c diabetes highlights the importance of early diagnosis, timely treatment, and preventive lifestyle choices.
The good news is that with proper medical care and healthy habits, many of these complications can be avoided or minimized—protecting not just pancreatic health, but overall metabolic well-being.
Takeaway: Understanding the Gallstone-Pancreas-Diabetes Connection
In summary, gallstones do far more than cause discomfort—they can obstruct the pancreatic duct, leading to pancreatitis.
This inflammation damages insulin-producing cells, resulting in Type 3c diabetes.
While lifestyle changes and medical treatments may help, understanding the risk of gallstones and their potential to lead to pancreatic inflammation and diabetes is vital.
Real-life cases like those of Emily, James, and Sarah show how gallstones, left untreated, can lead to significant and lasting damage to pancreatic function.
As research continues, the link between gallstones, pancreatic inflammation, and Type 3c diabetes grows stronger, urging individuals to recognize and address gallstone symptoms early.
References: