How Family History Increases Your Risk of Contracting Type 2 Diabetes?
- admin
- October 9, 2024
- 8:34 pm
- No Comments

When I first discovered that my grandmother had diabetes, I did not think much of it. I figured it was just one of those things that happened to older people.
Fast forward to my late 30s, and I found myself in my doctor’s office being warned about my own risk for type 2 diabetes.
It was a sobering wake-up call. What I did not realize back then, but now understand all too well, is that a family history of diabetes can significantly increase the chances of developing the disease.
This article by bestdietarysupplementfordiabetics.com will walk you through how and why that happens, based on both personal experience and scientific evidence.
Points Covered in This Article:
- The Genetic Connection: Why Family History Matters
- Lifestyle Choices Passed Down the Family Tree
- Environmental Factors Linked to Family History
- Scientific Evidence on Family History and Diabetes Risk
- Daily Lifestyle Habits that Worsen the Risk
- Can You Outsmart Your Genes?
- FAQs on Impact of Family History on Type 2 Diabetes
- Conclusion: Understanding the Weight of Family History
The Genetic Connection: Why Family History Matters
You’ve likely heard people talk about having a “family history of diabetes mellitus,” but what does that really mean?
Is it just bad luck, or is there more to it? Turns out, it is a mix of both.
The genetic link between family history and type 2 diabetes is strong, and this is something I personally experienced.
Researchers have identified several genes that contribute to the risk of developing type 2 diabetes.
For instance, variations in genes like TCF7L2 and FTO have been shown to increase diabetes susceptibility. If your parents or grandparents had these genetic variations, there is a good chance you could inherit them, raising your risk significantly.
According to the American Diabetes Association, if both parents have type 2 diabetes, the likelihood that their children will develop the condition can rise to 50%.
So, in a way, the risk of type 2 diabetes with family history is like playing a game of cards—except your deck might be stacked against you from the start.
Lifestyle Choices Passed Down the Family Tree
While genetics play a critical role, lifestyle is another powerful factor that often runs in families. It is not just your grandmother’s casserole recipe that gets handed down—habits around food (such as low carb diets), physical activity, and stress management are often passed on, too.
In my own family, weekend dinners were always a carb-heavy affair, loaded with pasta, bread, and sugary desserts. It was a way to bond, but over time, those habits took a toll.
I noticed that many of my relatives were overweight, and when I was diagnosed as prediabetic, I saw the connection.
The British Medical Journal published a study showing that family history of type 2 diabetes often leads to similar dietary patterns, which worsen the genetic predisposition.
If your family enjoys high-calorie, low-nutrient foods, lack of optimal hydration, the risk of developing type 2 diabetes increases dramatically.
Environmental Factors Linked to Family History
It is not just genetics or what is on your plate—the environment you grow up in can quietly shape your long-term health in powerful ways.
In families with a history of type 2 diabetes, it is common to see not just a genetic predisposition, but also a lifestyle blueprint that unknowingly reinforces unhealthy habits.
Sedentary behaviors tend to run in households where physical activity is not a norm. A 2023 study in The Lancet Diabetes & Endocrinology highlights that children from families with low physical activity levels are twice as likely to develop insulin resistance by their teenage years, even when controlling for BMI.
That is huge! It means inactivity itself—not just weight—can independently raise your risk.
Let’s get personal: my childhood was full of couch time and comfort food. We did not go on bike rides or weekend hikes.
Our “activity” was often limited to changing the TV channel. By the time I was 30, my waistline had expanded, and so had my blood sugar levels.
The connection between my sedentary upbringing and my escalating risk for type 2 diabetes hit me like a wake-up call.
Recent research from Diabetologia also confirms that family environments influence dietary patterns. Children raised in households with frequent consumption of high-sugar, high-fat foods are more likely to replicate those choices later in life.
Add in minimal exercise, and you have got a metabolic storm waiting to happen.
In short, even if your genes load the gun, your environment pulls the trigger. Recognizing these early influences can be empowering.
It gives you the chance to rewrite your habits and reduce your risk—regardless of what is in your DNA.
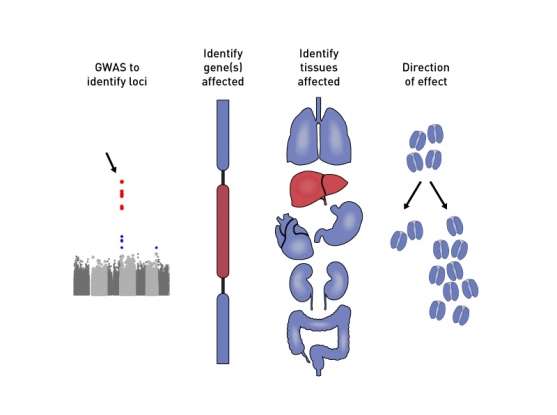
Scientific Evidence on Family History and Diabetes Risk
Science supports the link between family history and type 2 diabetes risk.
Studies, like the one conducted by the Diabetes Prevention Program Research Group, have demonstrated that individuals with a family history of diabetes have a 2 to 3 times higher risk of developing the condition compared to those without such a history.
Furthermore, the Framingham Heart Study, one of the longest-running cohort studies, revealed that even with moderate lifestyle changes, the inherited risk is hard to completely avoid.
People with a family history of diabetes type 2 who maintain a healthy lifestyle are still at a higher risk compared to those with no family history, proving that genetics are a key player.
Daily Lifestyle Habits that Worsen the Risk
There is no denying that your family history sets the stage, but daily habits often take center stage.
I learned this the hard way. With a job that kept me tied to a desk and a love for sugary snacks, I was unknowingly pushing myself closer to a diabetes diagnosis, thanks to my genetic predisposition.
Some of the worst offenders include a lack of physical activity, poor diet, and high levels of stress. People with a family history of diabetes type 2 often fall into similar routines because these behaviors are normalized within the family structure.
It is not uncommon to see entire families struggle with weight management and stress, further increasing their chances of developing type 2 diabetes.
Research from The Lancet highlights that even in genetically predisposed individuals, adopting better habits can delay or prevent the onset of the disease.
But if those habits are not addressed, the combination of poor lifestyle and a family history of diabetes type 2 creates a perfect storm for developing the condition.
Can You Outsmart Your Genes?
So, what if your family history seems to be working against you?
Can you outsmart your genes?
The short answer is: “sort of”.
While you can’t change your genetic makeup, you can modify your environment and habits to reduce the risk.
For example, one simple change that had a huge impact on my life was swapping out sugary snacks for whole foods like fruits and nuts.
I also took up regular walking, which studies have shown can lower insulin resistance—an early precursor to diabetes.
A 2017 study in the Journal of Clinical Endocrinology & Metabolism demonstrated that moderate-intensity exercise helps improve glucose metabolism, even in people with a family history of diabetes how to prevent such risks.
The idea here is not to fight your genes but to work with them by adopting a lifestyle that reduces the chances of those genetic triggers being pulled.
FAQs on Impact of Family History on Type 2 Diabetes:
Q-1: How does family history increase the risk of type 2 diabetes in adults?
A: Family history significantly increases the risk of developing type 2 diabetes due to both genetic and shared lifestyle factors. In the United States, about 11.6% of the population (over 38 million people) live with diabetes, and most cases are type 2.
If close relatives have the condition, individuals may inherit genes that affect insulin function and glucose metabolism. Additionally, families often share dietary habits and activity levels, which can further increase risk.
Q-2: What is the percentage risk of type 2 diabetes if parents have it?
A: Risk increases notably when parents have type 2 diabetes. If one parent has the condition, the risk rises to approximately 30–40%, and if both parents are affected, it can increase to nearly 70%. In the United States, this makes family history one of the strongest predictors of future diabetes risk, especially when combined with lifestyle factors like poor diet and inactivity.
Q-3: What is the difference between genetic and lifestyle factors in type 2 diabetes?
A: Genetic factors determine susceptibility, while lifestyle factors influence whether the disease develops. In the United States, research shows that over 80% of type 2 diabetes cases are linked to lifestyle factors such as obesity and lack of exercise. However, individuals with a family history are more sensitive to these triggers, meaning unhealthy habits can lead to earlier onset of the disease.
Q-4: Can you prevent type 2 diabetes if it runs in your family?
A: Yes, prevention is possible even with a strong family history. Studies in the United States show that lifestyle changes can reduce the risk by up to 58%. Maintaining a healthy weight, exercising regularly, and eating a balanced Whole30 diet are key strategies. Early intervention is especially important for individuals with genetic risk factors.
Q-5: What is the risk of developing type 2 diabetes with one diabetic parent?
A: Having one diabetic parent increases the likelihood of developing the condition by about 2 to 4 times compared to individuals without a family history. In the United States, this elevated risk highlights the importance of regular health screenings and proactive lifestyle changes to delay or prevent onset.
Q-6: How hereditary is type 2 diabetes in the United States population?
A: Type 2 diabetes has a strong hereditary component, but it is not purely genetic. In the United States, family history is present in a large proportion of cases, yet environmental and behavioral factors play a major role. This means that while genes increase susceptibility, lifestyle choices ultimately determine outcomes.
Q-7: Does having siblings with type 2 diabetes increase your risk significantly?
A: Yes, having a sibling with type 2 diabetes can increase your risk by approximately 2–3 times. In the United States, shared environments and similar lifestyle patterns among siblings contribute to this elevated risk. Monitoring health markers like blood sugar levels becomes especially important in such cases.
Q-8: What are the early signs of type 2 diabetes in people with a family history?
A: Early signs include increased thirst, frequent urination, fatigue, blurred vision, and slow-healing wounds. In the United States, millions of people have prediabetes without knowing it. Individuals with a family history should be particularly vigilant, as early detection can prevent progression to full diabetes.
Q-9: How do family history and obesity together increase diabetes risk?
A: When combined, family history and obesity significantly amplify the risk of type 2 diabetes. In the United States, over 42% of adults are classified as obese, which is a major contributing factor. Excess body fat, especially around the abdomen, worsens insulin resistance, making it more likely for genetically predisposed individuals to develop the condition.
Q-10: What are the screening guidelines for type 2 diabetes if family history is present?
A: In the United States, adults with a family history of diabetes are advised to begin screening earlier than the general population, often starting at age 35 or sooner if additional risk factors are present. Regular screening every 1–3 years can help detect prediabetes or diabetes early, allowing for timely intervention and better health outcomes.
Understanding the Weight of Family History
In summary, family history plays a significant role in increasing your risk of type 2 diabetes. From inherited genes to shared lifestyle habits, your family can unknowingly set you up for a future struggle with the disease.
As someone who has faced the realities of a family history of type 2 diabetes, I can say that understanding the risk is crucial. Once you know what you are up against, you can take proactive steps to manage it.
But is family history a life sentence?
No.
While you cannot change your genetic predisposition, you can take control of your lifestyle choices to mitigate those risks.
Simple actions like adopting a healthier diet, increasing physical activity, and managing stress via behavioral therapy can go a long way in reducing your risk of diabetes type 2 family history or at least delaying its onset.
As the American Journal of Clinical Nutrition puts it, prevention through lifestyle modification is your best defense, even when your genetics are stacked against you.
By learning about herbs that lower blood sugar fast, you can outsmart your genes.